About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。


This is a significant study published in "The Lancet Gastroenterology & Hepatology" by a research team from the National Cancer Center, the National Cancer Clinical Medicine Research Center, and the Cancer Hospital of Peking Union Medical College, Chinese Academy of Medical Sciences in 2024.

Overview of the illness

Disease Interpretation
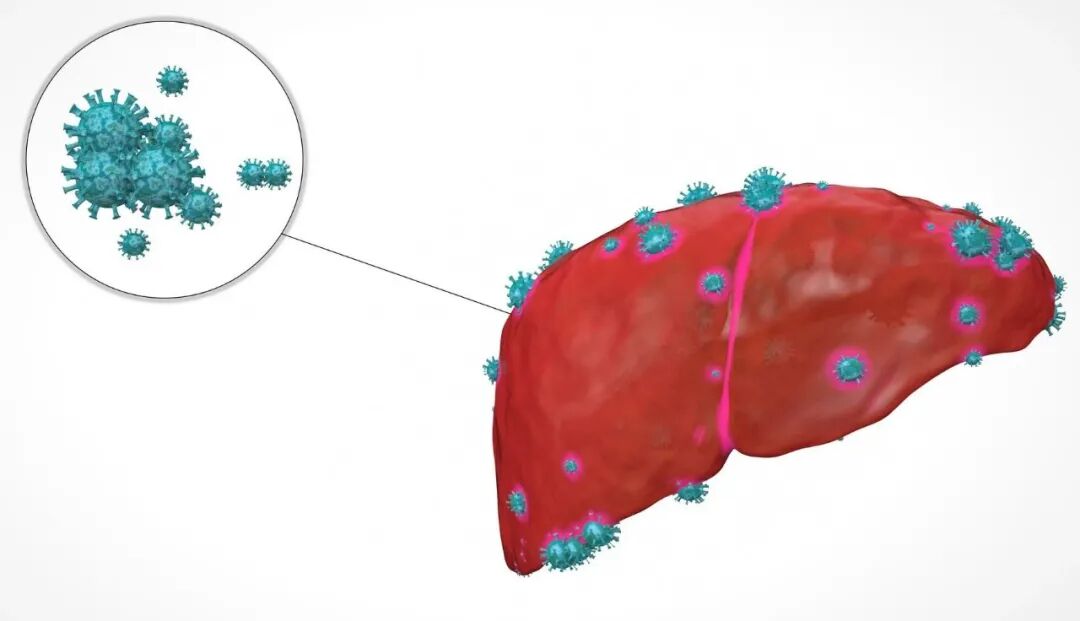
Imaging changes
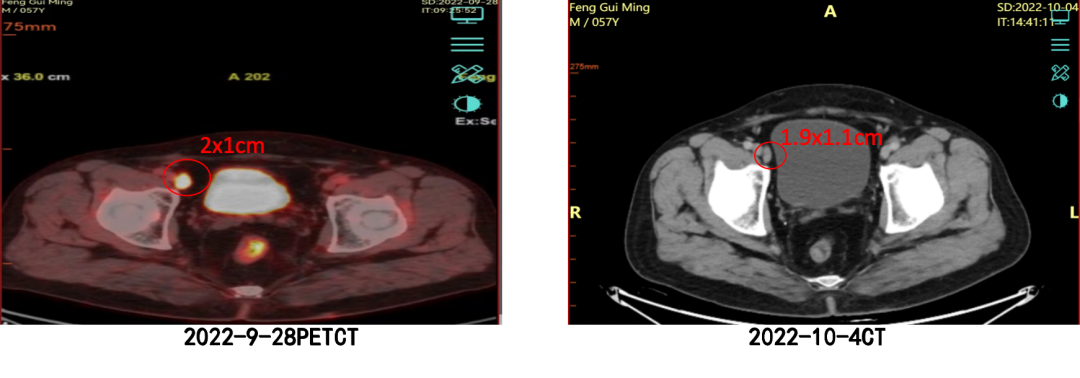
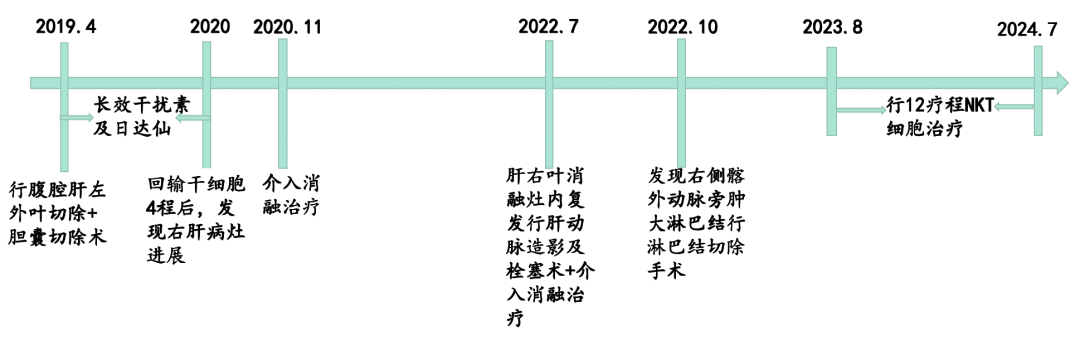
Conclusion and Review< H228>
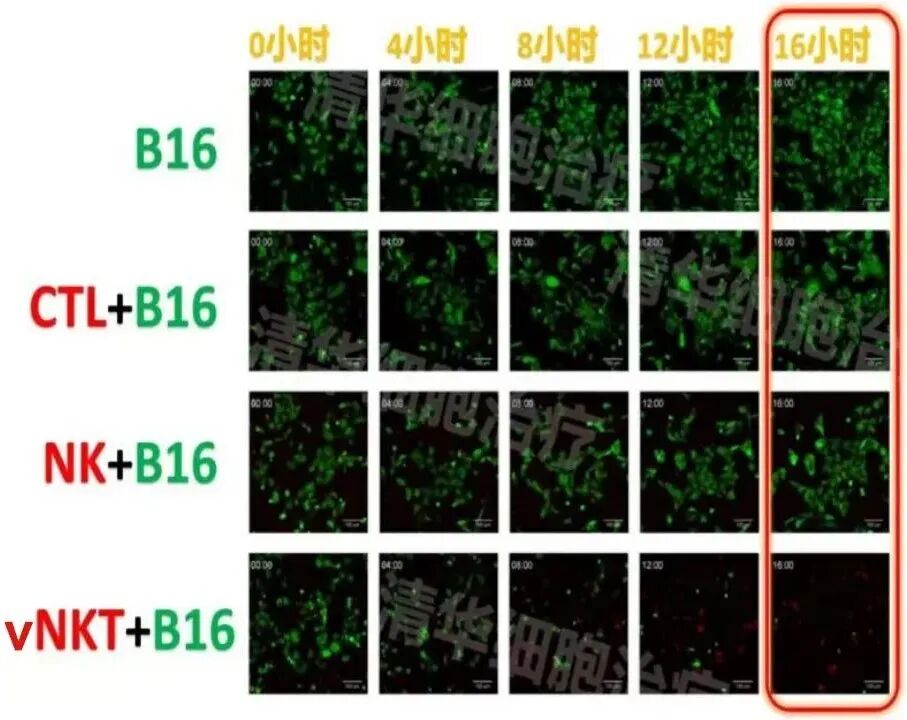
Experimental conditions: In the presence of vNKT cells, after 16 hours, nearly all B16 tumor cells were killed!

Founder of Lehe New Medicine
Professor Zhang Minghui, who holds a PhD in Immunology from Tsinghua University School of Medicine, has led a research team for over 20 years since the discovery of vNKT cells in 2002. They have accumulated experience in treating over 700 cases of solid tumors, covering almost all common solid tumors. The research results fully demonstrate the great value of vNKT cells in the treatment of solid tumors.

It is suitable for postoperative patients with high pathological malignancy or a risk of recurrence; patients whose tumors have been basically controlled but not cured through conventional treatments such as chemotherapy, radiotherapy, and targeted therapy; patients with persistent high carcinogenic factors; and patients intolerant to radiotherapy and chemotherapy. If these patients do not receive effective follow-up treatment after traditional anti-tumor therapy, recurrence, metastasis, or reoccurrence of tumors will be highly probable. In this case, vNKT cell therapy is an ideal follow-up treatment method that can significantly improve patient prognosis.

Scan QR code
Communicate with Professor Zhang Minghui's team
Click on the image to view the exciting content from previous issues